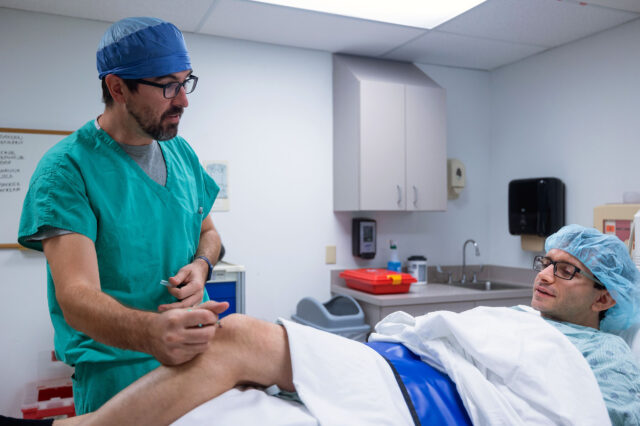
The UF Health Pain Management Center in Jacksonville is a comprehensive, multidisciplinary program to help patients cope with the debilitating effects of pain.
The center offers a full range of services for the evaluation, diagnosis and management of acute, chronic or cancer pain. The team of UF physicians is committed to providing expert treatment in a caring, comfortable, and patient-focused setting.
Treatment may include medications, therapeutic injections, physical therapy, psychological counseling, medical or surgical referral and patient education about pain management plan. We offer the full scope of services in modern pain management.